(Redirected from Denver Developmental Screening Test)
- Denver Developmental Screening Test Youtube Video
- Denver Developmental Screening Test Ii
- Denver Developmental Screening Test Cdc
| Denver Developmental Screening Tests | |
|---|---|
| Medical diagnostics | |
| Purpose | identify young children with developmental issues |
The Denver Developmental Screening Test was introduced in 1967 to identify young children, up to age six, with developmental problems. A revised version, Denver II, was released in 1992 to provide needed improvements. The purpose of the tests is to identify young children with developmental problems so that they can be referred for help.
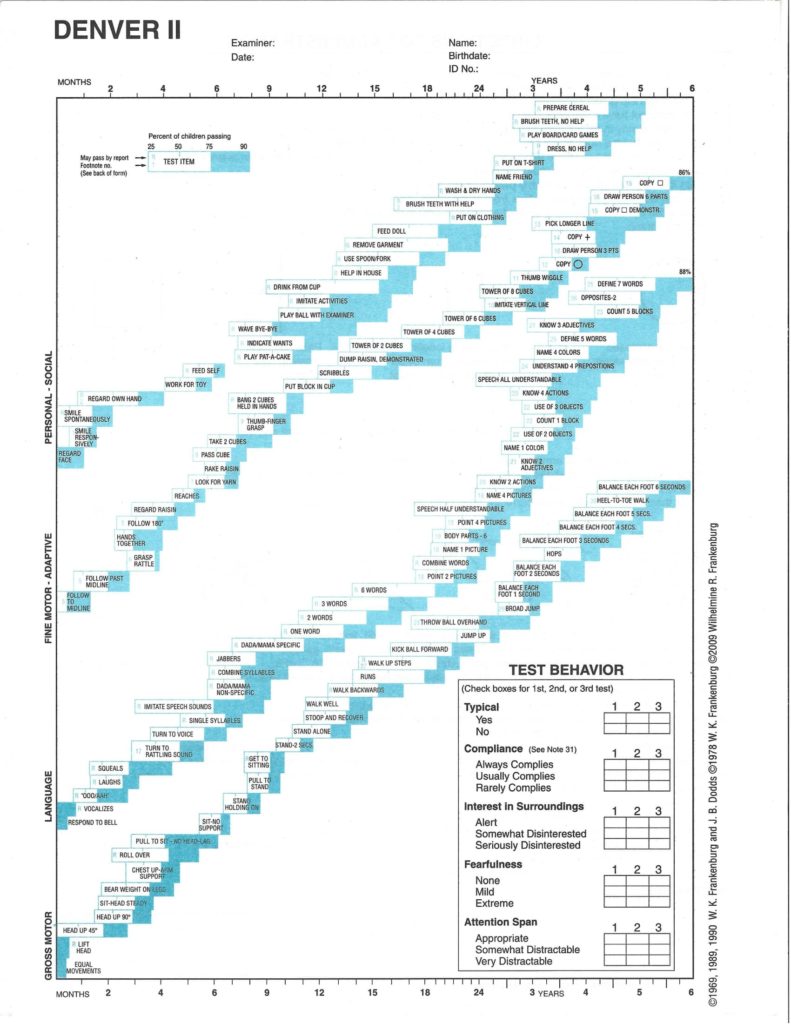
The tests address four domains of child development: personal-social (for example, waves bye-bye), fine motor and adaptive (puts block in cup), language (combines words), and gross motor (hops). They are meant to be used by medical assistants or other trained workers in programs serving children. Both tests differ from other common developmental screening tests in that the examiner directly tests the child. This is a strength if parents communicate poorly or are poor observers or reporters. Other tools, for example the Age and Stages Questionnaires, depend on parent report.
- 2Denver II
Denver Developmental Screening Test[edit]
The test was developed in Denver, Colorado, by Frankenburg and Dodds.[1] As the first tool used for developmental screening in normal situations like pediatric well-child care, the test became widely known and was used in 54 countries and standardized in 15.[2] The Denver Developmental Screening Test was published in 1967. During its first 25 years of use, one study found it to be insensitive to language delays.[3] Other concerns arose: that norms might vary by ethnic group or mother's education, that norms might have changed, and that users needed training.
Denver II[edit]
Research Basis[edit]
The Denver Developmental Screening Test was revised in order to increase its detection of language delays, replace items found difficult to use, and address the other concerns listed.[4] There are 125 items over the age range from birth to six years. An examiner administers the age-appropriate items to the child, although some can be passed by parental report. Each item is scored as pass, fail, or refused. Items that can be completed by 75%-90% of children but are failed are called cautions; those that can be completed by 90% of children but are failed are called delays. A normal score means no delay in any domain and no more than one caution; a suspect score means one or more delays or two or more cautions; a score of untestable means enough refused items that the score would be suspect if they had been delays. The Denver II is available in English and Spanish. Videotapes and two manuals describe 14 hours of structured instruction and recommend testing a dozen children for practice. Beyond this a professional degree is not required. As with all developmental testing, one must follow the instructions in detail.
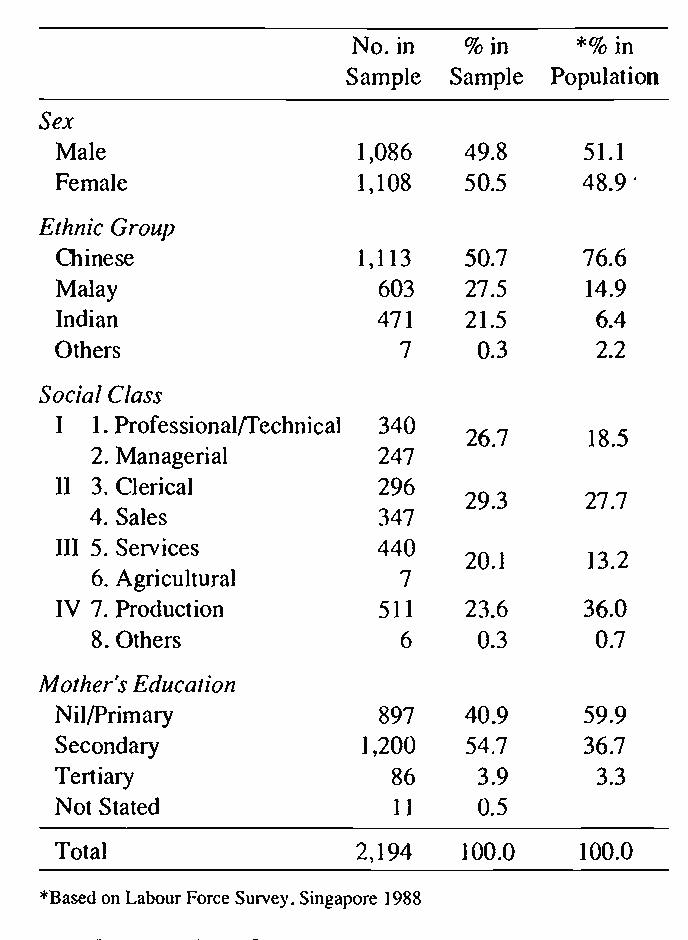
The standardization sample of 2,096 children was selected to represent the children of the state of Colorado. The test has been criticized because that population is slightly different from that of the U.S. as a whole. However, the authors found no clinically significant differences when results were weighted to reflect the distribution of demographic factors in the whole U.S. population. Significant differences were defined as differences of more than 10% in the age at which 90% of children could perform any given item [5]. Separate norms were provided for the 16 items whose scores varied by race, maternal education, or rural-urban residence.
Interpretation[edit]
The author of the test, William K. Frankenburg, likened it to a growth chart of height and weight and encouraged users to consider factors other than test results in working with an individual child. Such factors could include the parents’ education and opinions, the child’s health, family history, and available services. Frankenburg did not recommend criteria for referral; rather, he recommended that screening programs and communities review their results and decide whether they are satisfied. [6]
In 2006 the American Academy of Pediatrics Council on Children with Disabilities; Section on Developmental Behavioral Pediatrics published a list of screening tests for clinicians to consider when selecting a test to use in their practice. This list includes the DENVER II among its choices.[7] The chairman of the committee wrote: “In the practice of developmental screening and surveillance, we recommend the incorporation of parent-completed questionnaires or directly administered screening tests into the process of surveillance and screening. However, their results should be combined with attention to parental concerns and the pediatrician’s opinion, rather than replacing them, to augment the screening process and increase identification of children with developmental disorders”.[8]
Studies in Practice[edit]
One study evaluated the Denver II in terms of how its results matched those of a psychologist in five child-care centers: two serving the children of college-educated white parents and three serving low-income African-American children. The psychologist evaluated 104 children, of whom 18 were judged to be delayed [9]). All but two of the 18 came from the low-income centers but no mention is made regarding use of separate norms for African-American children. Results of the Denver II, using an older scoring method, included 33% questionable tests, in between normal and abnormal. If their scores were considered normal, too many children with delays would be missed (low sensitivity); if their scores were considered abnormal, too many children would be referred (low specificity). On the basis of this study, the Denver II fell into disfavor, and it is now seldom mentioned in reviews. Materials may no longer be purchased in hard copy, but they are available at no charge.
Another study evaluated the Denver II in the screening program of a community health center.[10] Here the criterion for abnormality was the eligibility of children for Early Intervention, according to the judgment of speech-language pathologists and other professionals in two suburban school districts. This study included 418 children in all and 64 who needed EI. The success of the screening program was judged in terms of predictive value: the probability that a child, if referred, would be eligible for services. The predictive value was 56%; allowing for children who were referred but not evaluated, it was 72%; this compared favorably with two studies using the Ages and Stages Questionnaire in clinics, which found comparable predictive values of 50% and 38%.[11] The study showed the value of taking into account other information besides the test result because the screener increased the predictive value from 44% to 56% by using her judgment not to refer some children with minor delays.
In a study of two-stage screening, children were prescreened with Frankenburg’s Revised Prescreening Developmental Questionnaire [12] and 421 with suspect scores were given the Denver II and evaluated by independent examiners.[13] In children under 18 months the prevalence of abnormality was 0.19 on diagnostic tests, and the Denver II had a positive predictive value of 0.36, a negative predictive value of 0.90, a sensitivity of 0.67, and a specificity of 0.72. The authors concluded that a suspect Denver II “should lead to careful monitoring and rescreening unless provider or parental concern suggests the need for immediate referral.” Among children 18–72 months old, the prevalence of abnormality was 0.43 and the positive predictive value of the Denver II was 0.77, negative predictive value of 0.89, sensitivity 0.86, and specificity of 0.81. The authors concluded that in their program a suspect Denver II should usually result in referral. (Positive predictive value meant the probability that a child with a suspect Denver II would be diagnosed as abnormal when evaluated; negative predictive value meant the probability that a child with a normal Denver II would be diagnosed as normal when evaluated.)
A study of 3389 children under five in Brazil has produced a continuous measure of child development for population studies.[14] The measure was based on the Denver Developmental Screening Test but can be used with the Denver II.
See also[edit]
- Child Development Stages,
- Developmental Disability,
- Early Childhood Intervention,
References[edit]
- ^Frankenburg, W.K. (1967). 'The Denver Developmental Screening Test'. The Journal of Pediatrics. 71 (2): 181–191. doi:10.1016/S0022-3476(67)80070-2.
- ^Frankenburg, W.K.; Dodds, J.; Archer, P. (1990). Denver II Technical Manual. Denver Developmental Materials, Inc. p. 1.
- ^Borowitz, K.C.; Glascoe, F.P. (1986). 'Sensitivity of the Denver Developmental Screening Test in Speech and Language Screening'. Pediatrics. 78: 1075–1078.
- ^Frankenburg, W.K.; Dodds, J.; Archer, P. (1990). Denver II Technical Manual. Denver Developmental Materials, Inc. p. 1.
- ^Frankenburg, W.K.; Dodds, J.; Archer, P. (1990). Denver II Technical Manual. Denver Developmental Materials, Inc. p. 6,18–19.
- ^Frankenburg, W.K.; Dodds, J.; Archer, P. (1990). Denver II Technical Manual. Denver Developmental Materials, Inc. p. 20–22.
- ^American Academy of Pediatrics, Council on Children with Disabilities; Section on Developmental Behavioral Pediatrics; Bright Futures Steering Committee; Medical Home Initiatives for Children with Special Needs Project Advisory Committee. Identifying infants and young children with developmental disorders in the medical home: an algorithm for developmental surveillance and screening. Pediatrics, 2006;118:405–420
- ^Lipkin, P.H.; Gwynn, H. (2007). 'Improving developmental screening: Combining parent and pediatrician opinions with standardized questionnaires'. Pediatrics. 119: 655–56.
- ^Glascoe, F.P.; Byrne, K.E.; Ashford, L.G. (1992). 'Accuracy of the Denver II in developmental screening'. Pediatrics. 89: 1221–1225.
- ^Dawson, P.; Camp, B.W. (2014). 'Evaluating developmental screening in clinical practice'. SAGE Open Medicine. 2: 205031211456257. doi:10.1177/2050312114562579. PMC4712749. PMID26770755.
- ^Guevara, J.P.; Gerdes, M.; Localio, R. (2013). 'Effectiveness of developmental screening in an urban setting'. Pediatrics. 131 (1): 30–37. doi:10.1542/peds.2012-0765. PMID23248223.
- ^Frankenburg, W.K. (1987). 'Revision of the Denver Prescreening Questionnaire'. J. Pediatr. 110: 653–57. doi:10.1016/S0022-3476(87)80573-5.
- ^Burgess, D.; Camp, B.W.; Spicer, C. (1996). 'Accuracy of the Denver II in a clinical developmental screening protocol'. Abstract Presented at the Society for Developmental-Behavioral Pediatrics.
- ^De Lourdes Drachler, M.; Marshall, T.; de Carvalho Leite, J.C. (2007). 'A continuous-scale measure of child development for population-based epidemiological surveys: A preliminary study using item-response theory for the Denver test'. Paediatric and Perinatal Epidemiology. 21 (2): 138–153. doi:10.1111/j.1365-3016.2007.00787.x. PMID17302643.
External links[edit]
- Developmental and Behavioral Pediatrics at American Academy of Pediatrics
- HealthyChildren.org American Academy of Pediatrics
Retrieved from 'https://en.wikipedia.org/w/index.php?title=Denver_Developmental_Screening_Tests&oldid=899868698'
The Denver Developmental Screening Test (DDST) is a test designed for use in initial screening of children to identify those with developmental problems so they can be referred for more precise evaluation and intervention, if appropriate. The test was developed and introduced in Denver, Colorado in the 1960s and is one of the most widely used developmental screening tests. Health care professionals can administer the test in clinical or office settings, and it takes between 10 and 20 minutes.
This test is intended for use in children between one month and six years of age. The exact age of the child is calculated so the administrator can select age-appropriate tasks designed to assess the child's personal and social skills, facility with language, fine motor skills, and gross motor skills. In addition to evaluating the child directly, the test administrator also asks the parents a series of questions to collect more information about how the child behaves at home.
If a child performs consistently below the standard of children in a similar age range, the Denver Developmental Screening Test will suggest the child may have a developmental problem. It is not designed to be specific, with lengthier and more detailed screening needed to evaluate children with test scores of concern. If a child performs at or above the expected level, the child is not considered to be at risk for developmental issues.
Also found in: Dictionary, Thesaurus, Legal, Financial, Acronyms, Encyclopedia, Wikipedia.
Related to Denver Developmental Screening Test: Developmental milestones
Denver Developmental Screening test
a test for identification of infants and preschool children with developmental delay.
Den·ver De·vel·op·men·tal Screen·ing Test
a scale used by psychologists and pediatricians to assess the developmental, intellectual, motor, and social maturity of children at any age level from birth to adolescence.
Denver Developmental Screening Test (DDST)
a test for evaluating development in children from 1 month to 6 years of age. The developmental level of motor, social, and language skills may be discovered by comparing the child's performance with the average performance of other children. The developmental age is expressed as a ratio in which the child's age is the denominator and the age at which the norm possesses skills equal to those of the child being tested is the numerator. The Denver II, released in 1990, is a major revision and restandardization of the DDST.
Denver developmental screening test
Psychology A screening test that assesses a child's neurodevelopmental maturation. See Psychological testing.Den·ver De·vel·op·men·tal Screen·ing Test
(DDS) (den'vĕr dĕ-vel'ŏp-men'tăl skrēn'ing test)A scale used by psychologists and pediatricians to assess the developmental, intellectual, motor, and social maturity of children from birth to age 6 years.
Want to thank TFD for its existence? Tell a friend about us, add a link to this page, or visit the webmaster's page for free fun content.
Link to this page:
Services on Demand
- text in Portuguese
- Cited by SciELO
Related links
- Similars in SciELO
Print version ISSN 1679-4508On-line version ISSN 2317-6385
http://dx.doi.org/10.1590/s1679-45082010ao1620 Original ArticleThe heart of The Sims is a leafy suburban neighborhood comprising pre-built houses of various size and value, along with several vacant lots to build new residences on. Die sims 1 free download vollversion deutsch. Indeed, at its core The Sims is a sort of virtual people farm of everyday life management.The concept at its foundation – the interactive simulation of a person’s everyday life and all that it entails – is ambitious in the extreme, and amazingly the design does it ample justice. Live The Way You WantThe Sims is essentially divided into two sections – a “Live” mode in which your Sims work, play, and interact, and a Buy/Build mode that freezes time to allow you to change the environment. The lives of the Sims under your control are faceted and detailed enough that, just like all of us in the PC Gamer office who have become curiously entranced, you’ll actually find yourself believing that you’re living somebody else’s life vicariously. Your Sim becomes a virtual alter-ego through which you can attempt to make real your dreams – or, perhaps, nightmares.Denver II: evaluation of the development of children treated in the outpatient clinic of Project Einstein in the Community of Paraisópolis1Master's degree in Nursing; Professor at Faculdade de Enfermagem of Hospital Israelita Albert Einstein – HIAE, São Paulo (SP), Brazil2Nurse; Specialist in Pediatric and Neonatal Nursing at Faculdade de Enfermagem of Hospital Israelita Albert Einstein – HIAE, São Paulo (SP), Brazil3Nurse; Specialist in Pediatric and Neonatal Nursing at Faculdade de Enfermagem of Hospital Israelita Albert Einstein – HIAE, São Paulo (SP), Brazil4PhD in Psychology; Professor at Faculdade de Enfermagem of Hospital Israelita Albert Einstein – HIAE, São Paulo (SP), BrazilObjectives:To evaluate the neuropsychomotor development of children treated in an outpatient clinic, using the Denver Developmental Screening Test II (DDST-R).Methods:This was an exploratory descriptive research using a quantitative approach, conducted in the outpatient clinic of the Project Einstein in the Community of Paraisopolis (PECP), São Paulo, Brazil. The sample consisted of 35 children, from birth to 6 years of age, most of them from 1 to 3 years old (19; 54.3%). They underwent the Denver II Test, which assesses four neuropsychomotor development areas: gross motor, fine motor adaptive, language and personal-social.Results:Most of the children (24, 68.6%) had test results compatible with normal development, while 10 (28.6%) had a “risk” test and 1 (2.9%) was “untestable” due to refusal to carry out the proposed activities. As to the items evaluated in each area, 7 children (20%) showed a developmental “delay” (when the child does not perform the activity passed by more than 90% of the children of his/her age) and 18 (51%) required “attention” (when the child does not perform the activity passed by 75 to 90% of the children of his/her age), predominantly in the language area.Conclusions:Although most of the children (68.6%) presented normal development in the test, we point out that in the remaining children (31.4%), the number of items classified as “delay” or “attention”, and tests classified as “risk” or “untestable” suggest impairment in neuropsychomotor development. We underscore the importance of the routine administration of the DDST-R for an early detection of developmental disabilities and thus establish primary prevention programs.Keywords: Child development; Primary health care; Developmental disabilitiesINTRODUCTIONIn a broader concept, the child development is understood as a process that starts during the intrauterine life and involves several aspects, such as physical growth, neurological maturation, and the construction of skills related to the behavior in the child's cognitive, social and affective domains. The child development involves the individual's ability to carry out increasingly complex functions and is influenced by several factors, thus being worthy of special attention from health and education professionals(1–3).Children from developing countries are exposed to some risks such as a high prevalence of diseases, being born of a high-risk and/or incomplete pregnancy, and living in adverse socioeconomic conditions, and these make them more likely to present growth and developmental delays(4–5). Studies show the influence of family income, birth weight and nutritional status on the occurrence of developmental delay in children(4,6).The task of identifying and following up children vulnerable to neuropsychomotor development delay confronts the complexity of the factors that lead to this delay, the inexistence of an efficient surveillance system, the failure to use adequate assessment tools for screening, and more(7).In an attempt to follow up the neuropsychomotor development of children from birth to six years of age, the Denver Developmental Screening Test (DDTT) was created. Designed by Frankenburg et al. in 1967, this is an instrument for the early detection of disorders of child development that assesses four areas/categories: the gross motor, fine motor adaptive, language and personal-social areas(1,8–12).Denver Developmental Screening Test Youtube Video
The motor behavior is associated with the maturation of the nervous system, corresponding to the control of motor acquisitions. The language behavior encompasses sound and image perceptions as well as their responses, whereas the adaptive behavior consists of the child's reactions to objects and situations. The personal-social behavior, in turn, corresponds to the evaluation of behavior in face of cultural stimuli(1,8–10).In 1990, the authors proposed a new version, known as Revised Denver Developmental Screening Test (DDST-R) or Denver II. Some language-related items were excluded and other items, which were difficult to administer or interpret, were modified or excluded. The test now consists of 125 items, and the manner of interpreting and administering the tasks and the test as a whole were also modified(1,4,9–10,12–13).We should point out that this instrument is not a test for the assessment of intelligence and development quotients, but it allows the assessment of the child's current maturational development status, and should not be used as a diagnostic tool(8,11).The data obtained by means of this test indicate whether the child is developing according to the expected for their chronological age and maturity, and provide information both for planning action strategies for the child and for advising parents(1,4,8–10).Among the tests used for the follow-up of child development, DDST-R is one of the most widely used, according to a bibliographic survey carried out in the past 25 years that analyzed 174 scientific articles(12).In the field of pediatric Nursing, this test is used as an effective strategy for collecting data on a child; these data are essential for the elaboration of nurse prescriptions, aiming at the integral care of both the child and their family(8).For being easy to use, DDST-R may be administered in basic health units, outpatient clinics, medical offices, clinics, in-hospital pediatric units, day-care centers, kindergartens, and services specialized in child development disorders. It allows each professional to read the data obtained in light of their specific background(8).The administration of DDST-R in pediatric outpatient clinics is of the utmost importance, since it is a primary care service aimed at promoting health, and thus contributes to the early detection of neuropsychomotor development deficits. In view of these facts, the objective of this study was to address the use of this instrument in the follow-up of the development of children treated in an outpatient clinic that cares for children of a slum in São Paulo, Brazil.OBJECTIVETo evaluate the neuropsychomotor development of children from birth to six years of age treated in an outpatient clinic, using the Denver Developmental Screening Test II (DDST-R).METHODSThis is an exploratory descriptive study using a quantitative approach, conducted in the outpatient clinic of Project Einstein in the Community of Paraisopolis (PECP), located in the city of São Paulo.Approximately 10 thousand children aged up to 10 years are treated in this clinic, where they receive free medical and hospital services, advice regarding use of the medications supplied, and multiple complementary initiatives in the health area(14).A total of 35 children from birth to six years of age regularly enrolled and treated in PECP participated in the study, with permission of their guardians who gave written informed consent. Most of the children were aged between 12 and 36 months (19; 54.3%) as shown in table 1.Table 1 Distribution of children submitted to the DDST-R per stage of development
| Stage of development | Children | |
|---|---|---|
| n | % | |
| Infant* | 5 | 14.3 |
| Toddler** | 19 | 54.3 |
| Pre-school*** | 11 | 31.4 |
| Total | 35 | 100 |
*Infant: children aged up to 12 months;
**Toddler: children aged from one to three years;
***Pre-school: children aged from three to six years.
Data collection occurred after approval of the research project by the Scientific Commission of the Nursing School of Hospital Israelita Albert Einstein and by the institutional Research Ethics Committee (CAAE: 0160.0.028.000-08); authorization was also obtained from the administration of the outpatient clinic where the data were collected. Kaze ga tsuyoku fuiteiru watch.
The data were collected in the second semester of 2008, by means of DDST-R administration, and the materials used were: a red woolen pompom with a thread; a rattle with a narrow handle; raisins; a small bell; ten 2.5-cm3 colored wooden blocks; a clear pot with narrow opening; a tennis ball; a red pencil; a small plastic doll with a toy baby bottle; a plastic mug with handles and blank paper(1).
Data were quantitatively analyzed using descriptive statistics, and expressed as absolute numbers and percentages, in the format of tables, considering the criteria of test result interpretation.
Denver Developmental Screening Test Ii
Each DDST-R item is correlated with the age and percentage of the standard population that performed one given item or behavior. Each of the items evaluated is classified as:

–. normal: when the child performs an activity expected for their age or does not perform an activity passed by less than 75% of the children of the same age;
–. attention: when the child does not perform or refuses to perform an activity passed by 75 to 90% of the children of the same age;
–. delay: when the child does not perform or refuses to perform an activity passed by more than 90% of the children of the same age(1,8–10,13).
According to the interpretation of the items, the test can be classified as: normal, when the child has no developmental “delay”, or requires attention, at most; risk, when the child's test has two or more items classified as requiring attention and/or one or more items showing developmental “delay”; and untestable, when the child “refuses” to perform the activity of one or more items with the age line completely to the right (i.e., activity passed by almost all children) or of more than one item with the age line in the area where 75 to 90% of the children pass that item(1,10,13).
RESULTS
The development of the majority of the children assessed (24; 68.5%) was compatible with their age range; the tests of 10 children (28.6%) was classified as “risk”, and only 1 (2.9%) was “untestable”.
Initially considering the number of children with “delays”, in a total of seven, we verified that these delays were more frequent in the “fine motor adaptive” category (3; 42%), followed by the “personal-social” (2; 28.6%) and “language” (2; 28.6%) categories. As for the number of delays identified, in a total of 10, half (5; 50%) occurred in the language area (Table 2).
Table 2 Number of children presenting “delay” and items detected as “delay” in application of the DDST-R, per area/category of the test*
| Areas/categories | Children presenting “delay” | Test items identified as “delay” | ||
|---|---|---|---|---|
| n | % | n | % | |
| Personal-social | 2 | 28.6 | 2 | 20 |
| Fine motor adaptative | 3 | 42.9 | 3 | 30 |
| Language | 2 | 28.6 | 5 | 50 |
| Gross motor | - | - | - | - |
| Total | 7 | 100 | 10 | 100 |
*Delay occurs when the child does not perform or refuses to perform an activity that is conducted by over 90% of children at the same age.
As regards the activities classified as requiring “attention”, in a total of 21 identified in 18 children, we verified that the language area was also the most frequently affected, both in relation to the number of children (7; 38.9%), and to the number of test items (9; 42.9%), as shown in table 3.
Table 3 Number of children presenting “attention” and items detected as “attention” in application of the DDST-R, per area/category of the test*
| Areas/categories | Children presenting “attention” | Test items identified as “attention” | ||
|---|---|---|---|---|
| n | % | n | % | |
| Personal-social | 6 | 33.3 | 7 | 33.3 |
| Fine motor adaptative | 5 | 27.8 | 5 | 23.8 |
| Language | 7 | 38.9 | 9 | 42.9 |
| Gross motor | - | - | - | - |
| Total | 18 | 100 | 21 | 100 |
*Attention occurs when the child does not perform or refuses to perform an activity that is conducted by 75 to 90% of children at the same age.
In relation to the only child (2.9%) who refused to perform some items of the test, we observed a slight predominance in items of the language area (2; 50%), as shown in table 4.
Table 4 Number of children presenting “refusal” in application of the DDST-R, per area/category of the test*
| Areas/categories | Children presenting “refusal” | |
|---|---|---|
| n | % | |
| Personal-social | - | - |
| Fine motor adaptative | 1 | 25 |
| Language | 2 | 50 |
| Gross motor | 1 | 25 |
| Total | 4 | 100 |
*Refusal occurs when the child refuses to perform an activity in one or more items conducted by over 90% of children at the same age, or in more than one item that 75 to 90% of children at the same age have already carried out.
DISCUSSION
The number of “delays” and tests defined as of “risk” among the assessed children corroborates the findings of previous studies as regards the cumulative effects of multiple risk factors that increase the probability of impaired child development(15–16).
Children from underdeveloped countries concentrate the vast majority of the possible causes that lead to developmental delays. We should point out that this study was conducted in the community of the second largest slum in the State of São Paulo. However, other variables such as maternal education, family size and father's job were not analyzed in the present study, but are also important predictors of the future development of the child(7).
Since the objective of outpatient clinics is to provide the population with primary care, encompassing different specialties of the health area, the routine administration of DDST-R would facilitate the follow-up of possible deficits found in the neuropsychomotor development of children, thus permitting the elaboration of intervention programs aimed at preventing disorders.
Based on the analysis of the results found in relation to “risk” tests or “untestable” children, we recommended that the DDST-R be repeated, preferably two weeks later, for a better assessment of the child.
In relation to the higher frequency of “delays” and “attention” in the language area, two studies conducted with children in day-care centers also showed the persistence of deficits in this domain, that become more prominent after three years of age. According to the authors, these results can be explained, among other factors, by the neurophysiological immaturity for language acquisition and mastering, and also by social stimuli, which are essential for linguistic patterns to develop(13,17).
Considering this situation, it is important to advise parents on the need to follow up their children's activities and stimulate their verbalization using strategies such as: speaking slowly and articulately, singing songs, reading children's stories, etc.
If “risk” tests persist, referral of the child to a specialized professional (speech therapist, psychologist, ENT physician, and others) should be considered as recommended in the literature(4), in order to identify other factors such as hearing loss or emotional problems that could be related to this insufficient performance.
CONCLUSIONS
In view of the results, we concluded that the majority of the children showed normal development; 1/4 had a “risk” test, and only 1 child was “untestable”. The highest number of items pointing to “delays” or “attention” among the activities performed by the children occurred in the language area.
Considering the number of children with “delays” or “attention”, the language area had a high prevalence of “attention” items, whereas more children showed “delays” in the fine motor adaptive area.
Study carried out at Project Einstein in the Community of Paraisopolis (PECP) of the Sociedade Beneficente Israelita Brasileira Albert Einstein – SBIBAE, São Paulo (SP), Brazil.
REFERENCES
1. Almeida FA. Desenvolvimento da criança. In: Farah OGD, Sá AC, organizadores. Psicologia aplicada à enfermagem. São Paulo: Manole; 2008. [ Links ]
2. Miranda LP, Resegue R, Figueiras ACM. A criança e o adolescente com problemas do desenvolvimento no ambulatório de pediatria. J Pediatr (Rio J). 2003;79(Supl 1):S33-S42. [ Links ]
Denver Developmental Screening Test Cdc
3. Marcondes E, Vaz FAC, Ramos JLA, Okay Y. Pediatria básica: pediatria geral e neonatal. 9a ed. São Paulo: Sarvier; 2002. [ Links ]
4. Biscegli TS, Polis LB, Santos LM, Vicentin M. Avaliação do estado nutricional e do desenvolvimento neuropsicomotor em crianças freqüentadoras de creche. Rev Paul Pediatr. 2007;25(4):337-42. [ Links ]
5. Halpern R, Giugliani ERJ, Victora CG, Barros FC, Horta BL. Fatores de risco para suspeita de atraso no desenvolvimento neuropsicomotor aos 12 meses de vida. Rev Chil Pediatr. 2002;73(5):529-39. [ Links ]
6. Halpern R, Barros ADJ, Matijasevich A, Santos IS, Victora CG, Barros FC. Estado de desenvolvimento aos 12 meses de idade de acordo com peso ao nascer e renda familiar: uma comparação de duas coortes de nascimentos no Brasil. Rep Public Health. 2008;24(Supl 3):S444-S450. [ Links ]
7. Halpern R, Barros FC, Horta BL, Victora CG. Desenvolvimento neuropsicomotor aos 12 meses de idade em uma coorte de base populacional no sul do Brasil: diferenciais conforme peso ao nascer e renda familiar. Rep Public Health. 1996;12(Supl.1):73:8. [ Links ]
8. Brêtas JRS, Silva MGB, Silva CV. A aplicação do teste de triagem do desenvolvimento de Denver pelo enfermeiro pediatra: relato de caso. Acta Paul. Enferm. 1995; 8(4):9-18. [ Links ]
9. Barness LA. Manual de diagnóstico físico pediátrico. São Paulo. McGraw-Hill. São Paulo; 2000. [ Links ]
10. Frankenburg WK, Dodds J, Archer P, Shapiro H, Bresnick B. DENVER II: training manual. 2nd ed. Denver, USA: Denver Developmental Materials; 1992. [ Links ]
11. Ribeiro CA, Borba RIH. Crescimento e desenvolvimento da criança. In: Santos L, Silva E. Creche e pré-escola: uma abordagem de saúde. São Paulo: Artes Médicas; 2004. [ Links ]
12. Santos RS, Araújo APQC, Porto MAS. Diagnóstico precoce de anormalidades no desenvolvimento em prematuros: instrumentos de avaliação. J Pediatr (Rio J). 2008;84(4):289-99. [ Links ]
13. Rezende AR, Beteli VC, Santos JLF. Avaliação de habilidades de linguagem e pessoal-sociais pelo Teste de Denver II em instituições de educação infantil. Acta Paul Enferm. 2005;18(1):56-63. [ Links ]
14. Programa Einstein na Comunidade de Paraisópolis [Internet]. Brasil: Sociedade Beneficente Israelita Brasileira [atualizada 2007; citado 2009 Fev 17]. Disponível em: http://www.einstein.br/portal2007 [ Links ]
15. Meisels JS, Wasik BA. Who should be served? Identifying children in need of early intervention. In: Shonkoff JP, Meisels SJ, editors. Handbook of early intervention. Cambridge: Cambridge University Press; 1990. p. 605-32. [ Links ]
16. Sameroff AJ, Seifer R, Barocas R, Zax M, Greenspan S. Intelligence quotient scores of 4-year-old children: social-environmental risk factors. Pediatrics. 1987:79(3):343-50. [ Links ]
17. Andrade CRF. Prevalência das desordens idiopáticas da fala e da linguagem em crianças de um a onze anos de idade. J Public Health.1997;31(5):495-501. [ Links ]
Received: February 12, 2010; Accepted: May 10, 2010
This is an Open Access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
